-
 Early Feasibility Study of a Hybrid Tissue-Engineered Mitral Valve in an Ovine Model
Early Feasibility Study of a Hybrid Tissue-Engineered Mitral Valve in an Ovine Model -
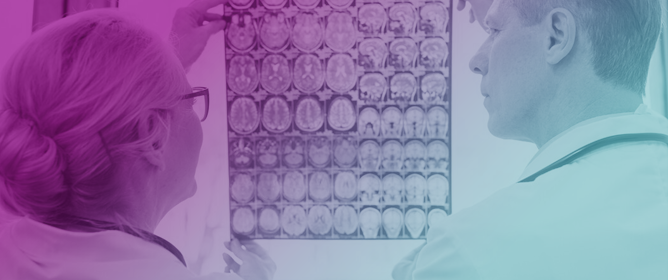 Thrombus Imaging Characteristics to Predict Early Recanalization in Anterior Circulation Large Vessel Occlusion Stroke
Thrombus Imaging Characteristics to Predict Early Recanalization in Anterior Circulation Large Vessel Occlusion Stroke -
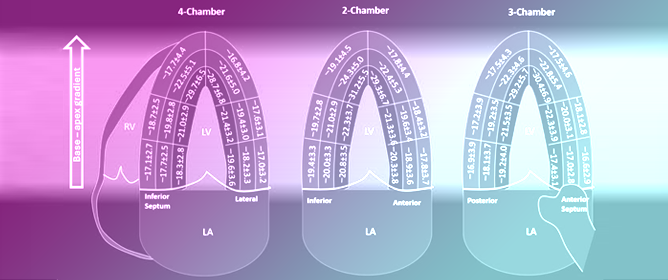 Lower Limit of Normality of Segmental Multilayer Longitudinal Strain in Healthy Adult Subjects
Lower Limit of Normality of Segmental Multilayer Longitudinal Strain in Healthy Adult Subjects -
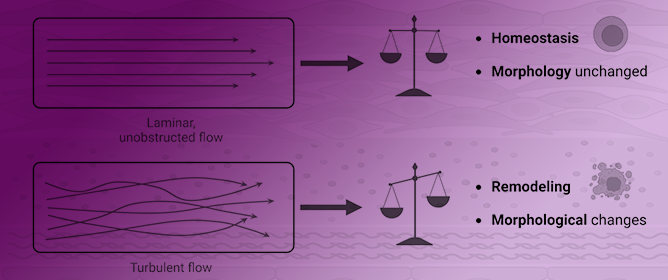 Aortic Valve Embryology, Mechanobiology, and Second Messenger Pathways: Implications for Clinical Practice
Aortic Valve Embryology, Mechanobiology, and Second Messenger Pathways: Implications for Clinical Practice
Journal Description
Journal of Cardiovascular Development and Disease
Journal of Cardiovascular Development and Disease
is an international, scientific, peer-reviewed, open access journal on cardiovascular medicine published monthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, CAPlus / SciFinder, and other databases.
- Journal Rank: CiteScore - Q2 (General Pharmacology, Toxicology and Pharmaceutics)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 20.3 days after submission; acceptance to publication is undertaken in 2.7 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
Impact Factor:
2.4 (2022);
5-Year Impact Factor:
3.0 (2022)
Latest Articles
Clinical Features and Patient Outcomes in Infective Endocarditis with Surgical Indication: A Single-Centre Experience
J. Cardiovasc. Dev. Dis. 2024, 11(5), 138; https://doi.org/10.3390/jcdd11050138 (registering DOI) - 29 Apr 2024
Abstract
Background: Infective endocarditis (IE) is marked by a heightened risk of embolic events (EEs), uncontrolled infection, or heart failure (HF). Methods: Patients with IE and surgical indication were enrolled from October 2015 to December 2018. The primary endpoint consisted of a composite of
[...] Read more.
Background: Infective endocarditis (IE) is marked by a heightened risk of embolic events (EEs), uncontrolled infection, or heart failure (HF). Methods: Patients with IE and surgical indication were enrolled from October 2015 to December 2018. The primary endpoint consisted of a composite of major adverse events (MAEs) including all-cause death, hospitalizations, and IE relapses. The secondary endpoint was all-cause death. Results: A total of 102 patients (66 ± 14 years) were enrolled: 50% with IE on prosthesis, 33% with IE-associated heart failure (IE-aHF), and 38.2% with EEs. IE-aHF and EEs were independently associated with MAEs (HR 1.9, 95% CI 1.1–3.4, p = 0.03 and HR 2.1, 95% CI 1.2–3.6, p = 0.01, respectively) and Kaplan–Meier survival curves confirmed a strong difference in MAE-free survival of patients with EEs and IE-aHF (p < 0.01 for both). IE-aHF (HR 4.3, 95% CI 1.4–13, p < 0.01), CRP at admission (HR 5.6, 95% CI 1.4–22.2, p = 0.01), LVEF (HR 0.9, 95% CI 0.9–1, p < 0.05), abscess (HR 3.5, 95% CI 1.2–10.6, p < 0.05), and prosthetic detachment (HR 4.6, 95% CI 1.5–14.1, p < 0.01) were independently associated with the all-cause death endpoint. Conclusions: IE-aHF and EEs were independently associated with MAEs. IE-aHF was also independently associated with the secondary endpoint.
Full article
(This article belongs to the Section Acquired Cardiovascular Disease)
Open AccessArticle
Epicardial Atrial Fat at Cardiac Magnetic Resonance Imaging and AF Recurrence after Transcatheter Ablation
by
Andrea Ballatore, Marco Gatti, Serena Mella, Davide Tore, Henri Xhakupi, Fabio Giorgino, Andrea Saglietto, Ludovica Carmagnola, Edoardo Roagna, Gaetano Maria De Ferrari, Riccardo Faletti and Matteo Anselmino
J. Cardiovasc. Dev. Dis. 2024, 11(5), 137; https://doi.org/10.3390/jcdd11050137 - 28 Apr 2024
Abstract
The relationship between epicardial adipose tissue (EAT) and atrial fibrillation (AF) has gained interest in recent years. The previous literature on the topic presents great heterogeneity, focusing especially on computed tomography imaging. The aim of the present study is to determine whether an
[...] Read more.
The relationship between epicardial adipose tissue (EAT) and atrial fibrillation (AF) has gained interest in recent years. The previous literature on the topic presents great heterogeneity, focusing especially on computed tomography imaging. The aim of the present study is to determine whether an increased volume of left atrial (LA) EAT evaluated at routine pre-procedural cardiac magnetic resonance imaging (MRI) relates to AF recurrences after catheter ablation. A total of 50 patients undergoing AF cryoballoon ablation and pre-procedural cardiac MRI allowing quantification of LA EAT were enrolled. In one patient, the segmentation of LA EAT could not be achieved. After a median follow-up of 16.0 months, AF recurrences occurred in 17 patients (34%). The absolute volume of EAT was not different in patients with and without AF recurrences (10.35 mL vs. 10.29 mL; p-value = 0.963), whereas the volume of EAT indexed on the LA volume (EATi) was lower, albeit non-statistically significant, in patients free from arrhythmias (12.77% vs. 14.06%; p-value = 0.467). The receiver operating characteristic curve testing the ability of LA EATi to predict AF recurrence after catheter ablation showed sub-optimal performance (AUC: 0.588). The finest identified cut-off of LA EATi was 10.65%, achieving a sensitivity of 0.5, a specificity of 0.82, a positive predictive value of 0.59 and a negative predictive value of 0.76. Patients with values of LA EATi lower than 10.65% showed greater survival, free from arrhythmias, than patients with values above this cut-off (84% vs. 48%; p-value = 0.04). In conclusion, EAT volume indexed on the LA volume evaluated at cardiac MRI emerges as a possible independent predictor of arrhythmia recurrence after AF cryoballoon ablation. Nevertheless, prospective studies are needed to confirm this finding and eventually sustain routine EAT evaluation in the management of patients undergoing AF catheter ablation.
Full article
(This article belongs to the Special Issue Modern Approach to Complex Arrhythmias)
►▼
Show Figures
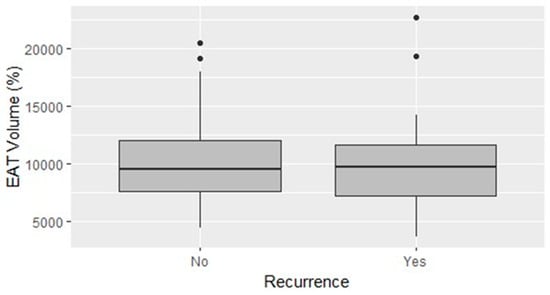
Figure 1
Open AccessArticle
Dementia Development during Long-Term Follow-Up after Surgical Aortic Valve Replacement with a Biological Prosthesis in a Geriatric Population
by
Ivo Deblier, Karl Dossche, Anthony Vanermen and Wilhelm Mistiaen
J. Cardiovasc. Dev. Dis. 2024, 11(5), 136; https://doi.org/10.3390/jcdd11050136 - 28 Apr 2024
Abstract
Surgical aortic valve replacement (SAVR) with a biological heart valve prosthesis (BHV) is often used as a treatment in elderly patients with symptomatic aortic valve disease. This age group is also at risk for the development of dementia in the years following SAVR.
[...] Read more.
Surgical aortic valve replacement (SAVR) with a biological heart valve prosthesis (BHV) is often used as a treatment in elderly patients with symptomatic aortic valve disease. This age group is also at risk for the development of dementia in the years following SAVR. The research question is “what are the predictors for the development of dementia?”. In 1500 patients undergoing SAVR with or without an associated procedure, preoperative (demographic, cardiac and non-cardiac comorbid conditions), perioperative (associated procedures, cross-clamp and cardiopulmonary bypass time) and postoperative 30-day adverse events (bleeding, thromboembolism, heart failure, conduction defects, arrhythmias, delirium, renal and pulmonary complications) were investigated for their effect on the occurrence of dementia by univariate analyses. Significant factors were entered in a multivariate analysis. The sum of the individual follow-up of the patients was 10,182 patient-years, with a mean follow-up of 6.8 years. Data for the development of dementia could be obtained in 1233 of the 1406 patients who left the hospital alive. Dementia during long-term follow-up developed in 216/1233 (17.2%) of the patients at 70 ± 37 months. Development of dementia reduced the mean survival from 123 (119–128) to 109 (102–116) months (p < 0.001). Postoperative delirium was the dominant predictor (OR = 3.55 with a 95%CI of 2.41–4.93; p < 0.00), followed by age > 80 years (2.38; 1.78–3.18; p < 0.001); preoperative atrial fibrillation (1.47; 1.07–2.01; p = 0.018); cardiopulmonary bypass time > 120 min (1.34; 1.02–1.78; p = 0.039) and postoperative thromboembolism (1.94; 1.02–3.70; p = 0.044). Postoperative delirium, as a marker for poor condition, and an age of 80 or more were the dominant predictors.
Full article
(This article belongs to the Section Cardiac Surgery)
►▼
Show Figures
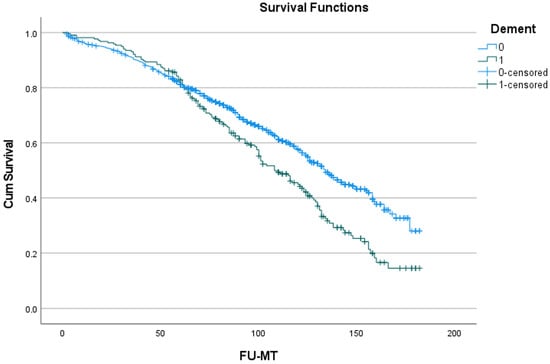
Figure 1
Open AccessSystematic Review
Klotho as an Early Marker of Acute Kidney Injury Following Cardiac Surgery: A Systematic Review
by
Konstantinos S. Mylonas, Panagiotis Karakitsos, Alireza Tajik, Deanna Pagliuso, Hamidreza Emadzadeh, Ioanna Soukouli, Pouya Hemmati, Dimitrios V. Avgerinos, George T. Stavridis and John N. Boletis
J. Cardiovasc. Dev. Dis. 2024, 11(5), 135; https://doi.org/10.3390/jcdd11050135 - 28 Apr 2024
Abstract
Acute kidney injury is a common complication following cardiac surgery (CSA-AKI). Serum creatinine levels require a minimum of 24–48 h to indicate renal injury. Nevertheless, early diagnosis remains critical for improving patient outcomes. A PRISMA-compliant systematic review of the PubMed and CENTRAL databases
[...] Read more.
Acute kidney injury is a common complication following cardiac surgery (CSA-AKI). Serum creatinine levels require a minimum of 24–48 h to indicate renal injury. Nevertheless, early diagnosis remains critical for improving patient outcomes. A PRISMA-compliant systematic review of the PubMed and CENTRAL databases was performed to assess the role of Klotho as a predictive biomarker for CSA-AKI (end-of-search date: 17 February 2024). An evidence quality assessment of the four included studies was performed with the Newcastle–Ottawa scale. Among the 234 patients studied, 119 (50.8%) developed CSA-AKI postoperatively. Serum Klotho levels above 120 U/L immediately postoperatively correlated with an area under the curve (AUC) of 0.806 and 90% sensitivity. Additionally, a postoperative serum creatinine to Klotho ratio above 0.695 showed 94.7% sensitivity and 87.5% specificity, with an AUC of 92.4%, maintaining its prognostic validity for up to three days. Urinary Klotho immunoreactivity was better maintained in samples obtained via direct catheterization rather than indwelling catheter collection bags. Storage at −80 °C was necessary for delayed testing. Optimal timing for both serum and urine Klotho measurements was from the end of cardiopulmonary bypass to the time of the first ICU lab tests. In conclusion, Klotho could be a promising biomarker for the early diagnosis of CSA-AKI. Standardization of measurement protocols and larger studies are needed to validate these findings.
Full article
(This article belongs to the Section Cardiac Surgery)
Open AccessBrief Report
Comparison of the Snare Loop Technique and the Hungaroring Reinforcement for Physician-Modified Endograft Fenestrations—An In Vitro Study
by
Artúr Hüttl, Tin Dat Nguyen, Sarolta Borzsák, András Süvegh, András Szentiványi, István Szilvácsku, Dóra Kovács, János Dobránszky, Péter Sótonyi and Csaba Csobay-Novák
J. Cardiovasc. Dev. Dis. 2024, 11(5), 134; https://doi.org/10.3390/jcdd11050134 - 25 Apr 2024
Abstract
►▼
Show Figures
Background: We conducted an in vitro comparison of the snare loop reinforcement against a closed-loop reinforcement (Hungaroring) for physician-modified endograft (PMEG) fenestrations regarding preparation time and stability during flaring balloon dilatation. Materials and methods: The time to complete a PMEG fenestration with reinforcement
[...] Read more.
Background: We conducted an in vitro comparison of the snare loop reinforcement against a closed-loop reinforcement (Hungaroring) for physician-modified endograft (PMEG) fenestrations regarding preparation time and stability during flaring balloon dilatation. Materials and methods: The time to complete a PMEG fenestration with reinforcement was measured and compared between the Hungaroring and snare loop groups. The number of stitches was counted. Each fenestration was dilated using a 10 mm high-pressure, non-compliant balloon up to 21 atm in pressure, and fluoroscopic images were taken. The presence of indentation on the oversized balloon at the level of the reinforcement was evaluated at each fenestration. Results: Five fenestrations were created in each group (n = 5) for a total of ten pieces. The completion time in the snare loop group was 1070 s (IQR:1010–1090) compared to 760 s (IQR:685–784) in the Hungaroring group (p = 0.008). Faster completion time was achieved by faster stitching (23.2 s/stitch (IQR 22.8–27.3) for the snare loop group and 17.3 s/stitch (IQR 17.3–20.1) for the Hungaroring group (p = 0.016). None of the fluoroscopic images of the snare loop reinforcement showed an indentation on the balloon during the overexpansion; on the contrary, the Hungaroring showed indentation in every case, even at 21 atm. Conclusion: Fenestrations reinforced with Hungaroring can be completed significantly faster. Furthermore, the Hungaroring resists over-dilation even at high pressures, while snare loop reinforcements dilate at nominal pressure.
Full article
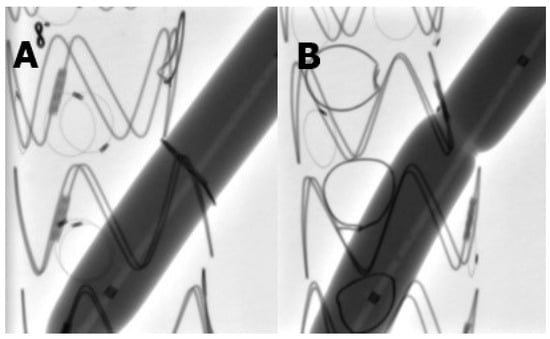
Figure 1
Open AccessArticle
Randomized Controlled Trial of Cardiac Rehabilitation Using the Balance Exercise Assist Robot in Older Adults with Cardiovascular Disease
by
Akihiro Hirashiki, Atsuya Shimizu, Takahiro Kamihara, Manabu Kokubo, Kakeru Hashimoto, Ikue Ueda, Kenji Sato, Koki Kawamura, Naoki Itoh, Toyoaki Murohara, Hitoshi Kagaya and Izumi Kondo
J. Cardiovasc. Dev. Dis. 2024, 11(5), 133; https://doi.org/10.3390/jcdd11050133 - 25 Apr 2024
Abstract
Background: Recent studies have investigated the effects of exercise on the functional capacity of older adults; training with a balance exercise assist robot (BEAR) effectively improves posture. This study compared the clinical safety and efficacy of training using BEAR video games to conventional
[...] Read more.
Background: Recent studies have investigated the effects of exercise on the functional capacity of older adults; training with a balance exercise assist robot (BEAR) effectively improves posture. This study compared the clinical safety and efficacy of training using BEAR video games to conventional resistance training in older adults with cardiovascular disease (CVD). Methods: Ninety patients (mean age: 78 years) hospitalized due to worsening CVD were randomized to cardiac rehabilitation (CR) Group R (conventional resistance training) or Group B (training using BEAR). After appropriate therapy, patients underwent laboratory testing and functional evaluation using the timed up-and-go test (TUG), short physical performance battery (SPPB), and functional independence measure (FIM) just before discharge and 4 months after CR. The rates of CVD readmission, cardiac death, and fall-related fractures were monitored. Results: BEAR had no adverse effects during exercise. At 4 months, TUG and SPPB improved significantly in both groups, with no significant difference between them. FIM motor and the Geriatric Nutritional Risk Index were significantly improved in Group B versus Group R. There was no significant difference in cardiac events and fall-related fractures between the two groups. Conclusion: CR with BEAR is safe and comparable to conventional resistance training for improving balance in older adults with CVD.
Full article
(This article belongs to the Special Issue Exercise and Cardiovascular Disease in Older Adults)
►▼
Show Figures
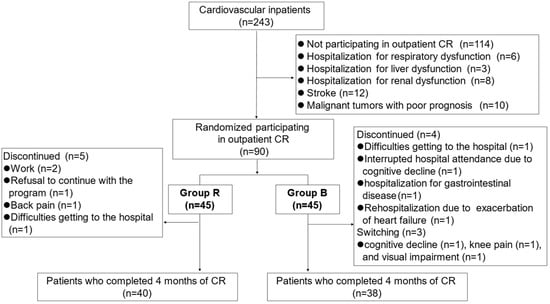
Figure 1
Open AccessArticle
Who Still Gets Ligated? Reasons for Persistence of Surgical Ligation of the Patent Ductus Arteriosus Following Availability of Transcatheter Device Occlusion for Premature Neonates
by
Julia K. Hoffmann, Zahra Khazal, Wievineke Apers, Puneet Sharma, Constance G. Weismann, Kira Kaganov, Craig R. Wheeler, Michael Farias, Diego Porras, Philip Levy and Sarah U. Morton
J. Cardiovasc. Dev. Dis. 2024, 11(5), 132; https://doi.org/10.3390/jcdd11050132 - 23 Apr 2024
Abstract
(1) Background: To identify reasons for the persistence of surgical ligation of the patent ductus arteriosus (PDA) in premature infants after the 2019 Food and Drug Administration (FDA) approval of transcatheter device closure; (2) Methods: We performed a 10-year (2014–2023) single-institution retrospective study
[...] Read more.
(1) Background: To identify reasons for the persistence of surgical ligation of the patent ductus arteriosus (PDA) in premature infants after the 2019 Food and Drug Administration (FDA) approval of transcatheter device closure; (2) Methods: We performed a 10-year (2014–2023) single-institution retrospective study of premature infants (<37 weeks) and compared clinical characteristics and neonatal morbidities between neonates that underwent surgical ligation before (epoch 1) and after (epoch 2) FDA approval of transcatheter closure; (3) Results: We identified 120 premature infants that underwent surgical ligation (n = 94 before, n = 26 after FDA approval). Unfavorable PDA morphology, active infection, and recent abdominal pathology were the most common reasons for surgical ligation over device occlusion in epoch 2. There were no differences in demographics, age at closure, or outcomes between infants who received surgical ligation in the two epochs; (4) Conclusions: Despite increasing trends for transcatheter PDA closure in premature infants, surgical ligation persists due to unfavorable ductal morphology, active infection, or abdominal pathology.
Full article
(This article belongs to the Special Issue Patent Ductus Arteriosus in Premature Babies)
►▼
Show Figures
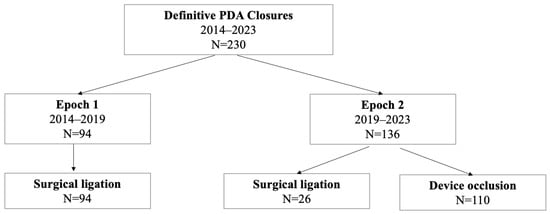
Figure 1
Open AccessSystematic Review
Associations of Atrioventricular Blocks and Other Arrhythmias in Patients with Lyme Carditis: A Systematic Review and Meta-Analysis
by
Nismat Javed, Eduard Sklyar and Jonathan N. Bella
J. Cardiovasc. Dev. Dis. 2024, 11(5), 131; https://doi.org/10.3390/jcdd11050131 - 23 Apr 2024
Abstract
►▼
Show Figures
Lyme disease often leads to cardiac injury and electrophysiological abnormalities. This study aimed to explore links between atrioventricular blocks and additional arrhythmias in Lyme carditis patients. This systematic review and meta-analysis of existing literature was performed from 1990 to 2023, and aimed to
[...] Read more.
Lyme disease often leads to cardiac injury and electrophysiological abnormalities. This study aimed to explore links between atrioventricular blocks and additional arrhythmias in Lyme carditis patients. This systematic review and meta-analysis of existing literature was performed from 1990 to 2023, and aimed to identify cases of Lyme carditis through serology or clinical diagnosis with concomitant arrhythmias. Pubmed and Web of Science were searched using appropriate MESH terms. Patients were divided into groups with atrioventricular blocks and other arrhythmias for cardiovascular (CV) outcome assessment. A total of 110 cases were analyzed. The majority (77.3%) were male, with mean age = 39.65 ± 14.80 years. Most patients presented within one week of symptom onset (30.9%). Men were more likely to have first-degree atrioventricular blocks (OR = 1.36 [95% CI 1.12–3.96], p = 0.01); these blocks tended to be reversible in nature (OR = 1.51 [95% CI 1.39–3.92], p = 0.01). Men exhibited a higher likelihood of experiencing variable arrhythmias (OR = 1.31 [95% CI 1.08–2.16], p < 0.001). Ventricular and supraventricular arrhythmias were more likely to exhibit instability (OR = 0.96 [95% CI 0.81–1.16] p = 0.01) and variability (OR = 1.99 [95% CI 0.47–8.31], p < 0.001). Men with Lyme carditis are likely to present with various atrioventricular blocks. These atrioventricular blocks are benign, and follow a predictable and stable clinical course. Further large-scale studies are warranted to confirm these associations.
Full article

Figure 1
Open AccessArticle
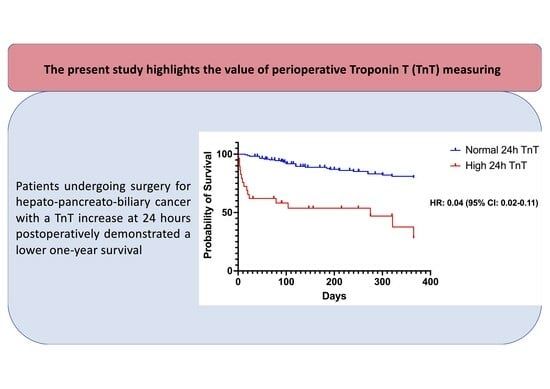
Validation of Perioperative Troponin Levels for Predicting Postoperative Mortality and Long-Term Survival in Patients Undergoing Surgery for Hepatobiliary and Pancreatic Cancer
by
Dimitrios E. Magouliotis, Evangelos Tatsios, Grigorios Giamouzis, Athina A. Samara, Andrew Xanthopoulos, Alexandros Briasoulis, John Skoularigis, Thanos Athanasiou, Metaxia Bareka, Christos Kourek and Dimitris Zacharoulis
J. Cardiovasc. Dev. Dis. 2024, 11(4), 130; https://doi.org/10.3390/jcdd11040130 - 22 Apr 2024
Abstract
Background: Hepatopancreato and biliary (HPB) tumors represent some of the leading cancer-related causes of death worldwide, with the majority of patients undergoing surgery in the context of a multimodal treatment strategy. Consequently, the implementation of an accurate risk stratification tool is crucial to
[...] Read more.
Background: Hepatopancreato and biliary (HPB) tumors represent some of the leading cancer-related causes of death worldwide, with the majority of patients undergoing surgery in the context of a multimodal treatment strategy. Consequently, the implementation of an accurate risk stratification tool is crucial to facilitate informed consent, along with clinical decision making, and to compare surgical outcomes among different healthcare providers for either service evaluation or clinical audit. Perioperative troponin levels have been proposed as a feasible and easy-to-use tool in order to evaluate the risk of postoperative myocardial injury and 30-day mortality. The purpose of the present study is to validate the perioperative troponin levels as a prognostic factor regarding postoperative myocardial injury and 30-day mortality in Greek adult patients undergoing HPB surgery. Method: In total, 195 patients undergoing surgery performed by a single surgical team in a single tertiary hospital (2020–2022) were included. Perioperative levels of troponin before surgery and at 24 and 48 h postoperatively were assessed. Model accuracy was assessed by observed-to-expected (O:E) ratios, and area under the receiver operating characteristic curve (AUC). Survival at one year postoperatively was compared between patients with high and normal TnT levels at 24 h postoperatively. Results: Thirteen patients (6.6%) died within 30 days of surgery. TnT levels at 24 h postoperatively were associated with excellent discrimination and provided the best-performing calibration. Patients with normal TnT levels at 24 h postoperatively were associated with higher long-term survival compared to those with high TnT levels. Conclusions: TnT at 24 h postoperatively is an efficient risk assessment tool that should be implemented in the perioperative pathway of patients undergoing surgery for HPB cancer.
Full article
(This article belongs to the Special Issue Epidemiology and Long-Term Outcomes in Cardiac Surgery, Thoracic Transplantation, and Interventional Cardiology)
►▼
Show Figures
Graphical abstract
Open AccessArticle
Prevalence and Clinical Significance of Intraventricular Conduction Disturbances in Hospitalized Children
by
Chiara Cirillo, Emanuele Monda, Raffaella Esposito, Diego Colonna, Cristina Falcone, Federica Irrissuto, Annapaola Cirillo, Adelaide Fusco, Federica Verrillo, Gaetano Diana, Marta Rubino, Martina Caiazza, Berardo Sarubbi, Giuseppe Limongelli and Maria Giovanna Russo
J. Cardiovasc. Dev. Dis. 2024, 11(4), 129; https://doi.org/10.3390/jcdd11040129 - 22 Apr 2024
Abstract
►▼
Show Figures
Introduction: Data on the prevalence and clinical significance of interventricular conduction disturbances (IVCDs) in children are scarce. While incomplete right bundle branch blocks (IRBBBs) seem to be the most frequent and benign findings, complete bundle blocks and fascicular blocks are often seen in
[...] Read more.
Introduction: Data on the prevalence and clinical significance of interventricular conduction disturbances (IVCDs) in children are scarce. While incomplete right bundle branch blocks (IRBBBs) seem to be the most frequent and benign findings, complete bundle blocks and fascicular blocks are often seen in children with congenital/acquired cardiac conditions. This study aims to delineate the prevalence and the diagnostic accuracy of IVCD in children admitted to a paediatric cardiology unit. Methods: Children admitted to the paediatric cardiology unit between January 2010 and December 2020 who had an ECG were included in the study. IVCDs were diagnosed according to standard criteria adjusted for age. Results: Three thousand nine hundred and ninety-three patients were enrolled. The median age was 3.1 years (IQR: 0.0–9.2 years), and 52.7% were males. IVCDs were present in 22.5% of the population: 17.4% of the population presented with IRBBBs, 4.8% with a complete right bundle branch block (CRBBB), 0.1% with a complete left bundle branch block (CLBBB), 0.2% with a left anterior fascicular block (LAFB) and 0.2% with a combination of CRBBB and LAFB. Also, 26% of children with congenital heart disease had an IVCD, and 18% of children with an IVCD had previous cardiac surgery. The overall sensitivity of IVCD in detecting a cardiac abnormality was 22.2%, with a specificity of 75.5%, a PPV of 83.1% and an NPV of 15.1%, but the values were higher for CLBBB and LAFB. Conclusions: IVCDs were present in one-fifth of children admitted to the cardiology unit. IRBBB was the most frequent disturbance, while CRBBB, CLBBB and fascicular blocks were much rarer, though they had a higher predictive value for cardiac abnormalities.
Full article
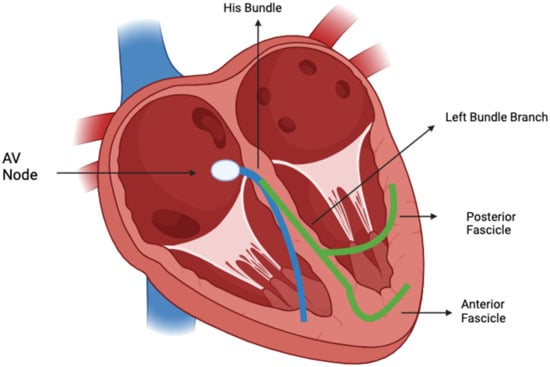
Figure 1
Open AccessArticle
Fasting Triglycerides in the Upper Normal Range Are Independently Associated with an Increased Risk of Diabetes Mortality in a Large Representative US Population
by
Yutang Wang
J. Cardiovasc. Dev. Dis. 2024, 11(4), 128; https://doi.org/10.3390/jcdd11040128 - 21 Apr 2024
Abstract
The association between normal-range triglyceride levels and diabetes mortality remains unclear. This cohort study aimed to elucidate this relationship by examining 19,010 US adult participants with fasting serum triglycerides below 150 mg/dL. Cox proportional hazards models were employed to estimate mortality hazard ratios
[...] Read more.
The association between normal-range triglyceride levels and diabetes mortality remains unclear. This cohort study aimed to elucidate this relationship by examining 19,010 US adult participants with fasting serum triglycerides below 150 mg/dL. Cox proportional hazards models were employed to estimate mortality hazard ratios (HRs) and 95% confidence intervals (CIs). Participants were followed up for a mean of 15.3 years, during which 342 diabetes deaths were recorded. A 1 natural log unit increase in triglycerides was associated with a 57% higher risk of diabetes mortality (adjusted HR, 1.57; 95% CI, 1.04–2.38). Comparable results were obtained when triglycerides were analyzed in quartiles. Receiver operating characteristic curve analysis identified an optimal triglyceride cutoff of 94.5 mg/dL for diabetes mortality; individuals with triglyceride levels above this threshold faced a greater risk of diabetes mortality (adjusted HR, 1.43; 95% CI, 1.12–1.83). Further investigation revealed a positive association between normal triglyceride levels and all-cause mortality, though no association was observed between normal triglycerides and mortality from hypertension or cardiovascular disease. In conclusion, elevated triglyceride levels within the normal range were associated with an increased risk of diabetes mortality. Individuals with triglyceride levels of 95 mg/dL or higher may require vigilant monitoring for diabetes and its associated complications.
Full article
(This article belongs to the Special Issue Cardiovascular Disease: Risk Factors and Prevention)
►▼
Show Figures
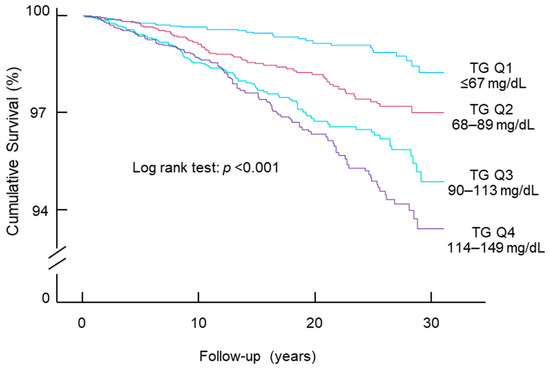
Figure 1
Open AccessReview
Photon-Counting Detector Computed Tomography (PCD-CT): A New Era for Cardiovascular Imaging? Current Status and Future Outlooks
by
Pietro G. Lacaita, Anna Luger, Felix Troger, Gerlig Widmann and Gudrun M. Feuchtner
J. Cardiovasc. Dev. Dis. 2024, 11(4), 127; https://doi.org/10.3390/jcdd11040127 - 21 Apr 2024
Abstract
Photon-counting detector computed tomography (PCD-CT) represents a revolutionary new generation of computed tomography (CT) for the imaging of patients with cardiovascular diseases. Since its commercial market introduction in 2021, numerous studies have identified advantages of this new technology in the field of cardiovascular
[...] Read more.
Photon-counting detector computed tomography (PCD-CT) represents a revolutionary new generation of computed tomography (CT) for the imaging of patients with cardiovascular diseases. Since its commercial market introduction in 2021, numerous studies have identified advantages of this new technology in the field of cardiovascular imaging, including improved image quality due to an enhanced contrast-to-noise ratio, superior spatial resolution, reduced artifacts, and a reduced radiation dose. The aim of this narrative review was to discuss the current scientific literature, and to find answers to the question of whether PCD-CT has yet led to a true step-change and significant progress in cardiovascular imaging.
Full article
(This article belongs to the Section Imaging)
►▼
Show Figures
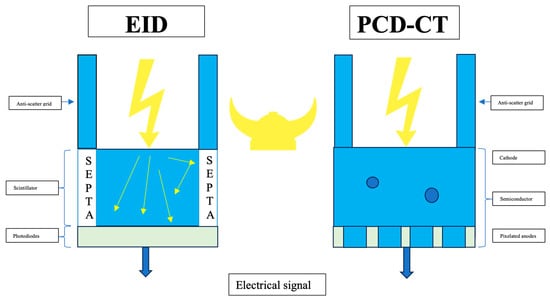
Figure 1
Open AccessReview
Atherosclerosis Residual Lipid Risk-Overview of Existing and Future Pharmacotherapies
by
Muntaser Omari and Mohammad Alkhalil
J. Cardiovasc. Dev. Dis. 2024, 11(4), 126; https://doi.org/10.3390/jcdd11040126 - 21 Apr 2024
Abstract
Patients with atherosclerotic disease remain at increased risk of future events despite receiving optimal medical treatment. This residual risk is widely heterogeneous, but lipoprotein particles and their content play a major role in determining future cardiovascular events. Beyond low-density lipoprotein cholesterol (LDL-c), other
[...] Read more.
Patients with atherosclerotic disease remain at increased risk of future events despite receiving optimal medical treatment. This residual risk is widely heterogeneous, but lipoprotein particles and their content play a major role in determining future cardiovascular events. Beyond low-density lipoprotein cholesterol (LDL-c), other lipoprotein particles have not demonstrated similar contribution to the progression of atherosclerosis. Statins, ezetimibe, and more recently, proprotein convertase subtilisin kexin 9 (PCSK9) inhibitors and bempedoic acid have confirmed the causal role of LDL-c in the development of atherosclerosis. Data on high-density lipoprotein cholesterol (HDL-c) suggested a possible causal role for atherosclerosis; nonetheless, HDL-c-raising treatments, including cholesteryl-ester transfer protein (CETP) inhibitors and niacin, failed to confirm this relationship. On the other hand, mendelian randomisation revealed that triglycerides are more implicated in the development of atherosclerosis. Although the use of highly purified eicosapentaenoic acid (EPA) was associated with a reduction in the risk of adverse cardiovascular events, this beneficial effect did not correlate with the reduction in triglycerides level and has not been consistent across large phase 3 trials. Moreover, other triglyceride-lowering treatments, such as fibrates, were not associated with a reduction in future cardiovascular risk. Studies assessing agents targeting angiopoietin-like 3 (lipoprotein lipase inhibitor) and apolipoprotein C3 antisense will add further insights into the role of triglycerides in atherosclerosis. Emerging lipid markers such as lipoprotein (a) and cholesterol efflux capacity may have a direct role in the progression of atherosclerosis. Targeting these biomarkers may provide incremental benefits in reducing cardiovascular risk when added to optimal medical treatment. This Review aims to assess available therapies for current lipid biomarkers and provide mechanistic insight into their potential role in reducing future cardiovascular risk.
Full article
(This article belongs to the Special Issue Dyslipidemia and Cardiovascular Disease: The Dawn of an Era with New Targets and Novel Therapies)
►▼
Show Figures
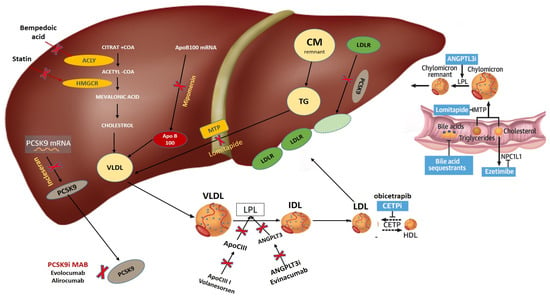
Figure 1
Open AccessReview
Novel Medical Treatments and Devices for the Management of Heart Failure with Reduced Ejection Fraction
by
Michele Alfieri, Filippo Bruscoli, Luca Di Vito, Federico Di Giusto, Giancarla Scalone, Procolo Marchese, Domenico Delfino, Simona Silenzi, Milena Martoni, Federico Guerra and Pierfrancesco Grossi
J. Cardiovasc. Dev. Dis. 2024, 11(4), 125; https://doi.org/10.3390/jcdd11040125 - 19 Apr 2024
Abstract
Heart failure (HF) is a growing issue in developed countries; it is often the result of underlying processes such as ischemia, hypertension, infiltrative diseases or even genetic abnormalities. The great majority of the affected patients present a reduced ejection fraction (≤40%), thereby falling
[...] Read more.
Heart failure (HF) is a growing issue in developed countries; it is often the result of underlying processes such as ischemia, hypertension, infiltrative diseases or even genetic abnormalities. The great majority of the affected patients present a reduced ejection fraction (≤40%), thereby falling under the name of “heart failure with reduced ejection fraction” (HFrEF). This condition represents a major threat for patients: it significantly affects life quality and carries an enormous burden on the whole healthcare system due to its high management costs. In the last decade, new medical treatments and devices have been developed in order to reduce HF hospitalizations and improve prognosis while reducing the overall mortality rate. Pharmacological therapy has significantly changed our perspective of this disease thanks to its ability of restoring ventricular function and reducing symptom severity, even in some dramatic contexts with an extensively diseased myocardium. Notably, medical therapy can sometimes be ineffective, and a tailored integration with device technologies is of pivotal importance. Not by chance, in recent years, cardiac implantable devices witnessed a significant improvement, thereby providing an irreplaceable resource for the management of HF. Some devices have the ability of assessing (CardioMEMS) or treating (ultrafiltration) fluid retention, while others recognize and treat life-threatening arrhythmias, even for a limited time frame (wearable cardioverter defibrillator). The present review article gives a comprehensive overview of the most recent and important findings that need to be considered in patients affected by HFrEF. Both novel medical treatments and devices are presented and discussed.
Full article
(This article belongs to the Special Issue Pathophysiology of HFpEF and HFrEF: Diagnosis, Mechanisms and Treatments)
►▼
Show Figures
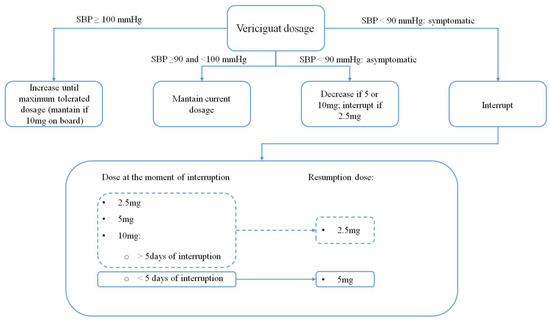
Figure 1
Open AccessArticle
Nitroprusside Combined with Leg Raise at the Time of Right Heart Catheterization to Differentiate Precapillary from Other Hemodynamic Forms of Pulmonary Hypertension: A Single-Center Pilot Study
by
Mostafa Naguib, Ahmed Aljwaid, Dean Marella, Raul J. Flores and Abhishek Singh
J. Cardiovasc. Dev. Dis. 2024, 11(4), 124; https://doi.org/10.3390/jcdd11040124 - 19 Apr 2024
Abstract
Pulmonary hypertension (PH) can arise from several distinct disease processes, with a percentage presenting with combined pre- and postcapillary pulmonary hypertension (cpcPH). Patients with cpcPH are unsuitable candidates for PH-directed therapies due to elevated pulmonary capillary wedge pressures (PCWPs); however, the PCWP is
[...] Read more.
Pulmonary hypertension (PH) can arise from several distinct disease processes, with a percentage presenting with combined pre- and postcapillary pulmonary hypertension (cpcPH). Patients with cpcPH are unsuitable candidates for PH-directed therapies due to elevated pulmonary capillary wedge pressures (PCWPs); however, the PCWP is dynamic and is affected by both preload and afterload. Many patients that are diagnosed with cpcPH are hypertensive at the time of right heart catheterization which has the potential to increase the PCWP and, therefore, mimic a more postcapillary-predominant phenotype. In this small pilot study, we examine the effect of nitroprusside combined with dynamic preload augmentation with a passive leg raise maneuver in hypertensive cpcPH patients at the time of right heart catheterization to identify a more precapillary-dominant PH phenotype. Patients that met the criteria of PCWP ≤ 15 mmHg with nitroprusside infusion and PCWP ≤ 18 mmHg with nitroprusside infusion and simultaneous leg raise were started on pulmonary vascular-targeted therapy. Long-term PH therapy was well tolerated, with increased six-minute walk distance, improved WHO functional class, decreased NT-proBNP, and improved REVEAL 2.0 Lite Risk Score in this precapillary-dominant PH phenotype. This small study highlights the importance of characterizing patient physiology beyond resting conditions at the time of right heart catheterization.
Full article
(This article belongs to the Special Issue Pulmonary Hypertension: Current Status of Diagnosis and Treatment)
►▼
Show Figures
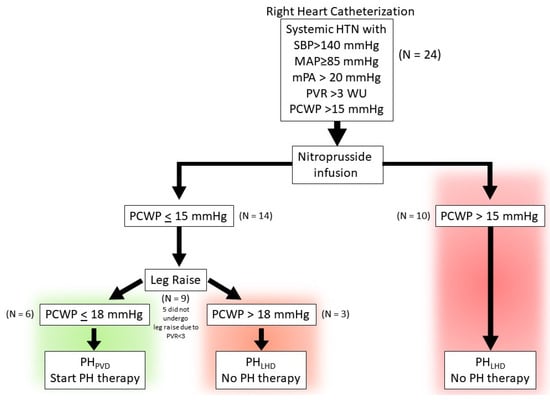
Figure 1
Open AccessArticle
Simplified Criteria for Identification of Familial Hypercholesterolemia in Children: Application in Real Life
by
Raffaele Buganza, Giulia Massini, Maria Donata Di Taranto, Giovanna Cardiero, Luisa de Sanctis and Ornella Guardamagna
J. Cardiovasc. Dev. Dis. 2024, 11(4), 123; https://doi.org/10.3390/jcdd11040123 - 17 Apr 2024
Abstract
Background: The diagnosis of familial hypercholesterolemia (FH) in children is primarily based on main criteria including low-density lipoprotein cholesterol (LDL-C) levels, increased in the proband and relatives, and its inheritance. Two other relevant parameters are symptoms, rarely occurring in children, as rare are
[...] Read more.
Background: The diagnosis of familial hypercholesterolemia (FH) in children is primarily based on main criteria including low-density lipoprotein cholesterol (LDL-C) levels, increased in the proband and relatives, and its inheritance. Two other relevant parameters are symptoms, rarely occurring in children, as rare are the FH homozygous patients, and the mutation detection of related genes. The latter allows the final diagnosis, although it is not commonly available. Moreover, the application of diagnostic scores, useful in adults, is poorly applied in children. The aim of this study was to compare the reliability of criteria here applied with different scores, apart from genetic analysis, for FH diagnosis. The latter was then confirmed by genetic analysis. Methods: n. 180 hypercholesterolemic children (age 10.2 ± 4.6 years) showing LDL-C levels ≥95th percentile (age- and sex-related), the dominant inheritance pattern of hypercholesterolemia (including LDL-C ≥95th percentile in one parent), were considered potentially affected by FH and included in the study. The molecular analysis of the LDLR, APOB and PCSK9 genes was applied to verify the diagnostic accuracy. Biochemical and family history data were also retrospectively categorized according to European Atherosclerosis Society (EAS), Simon Broome Register (SBR), Pediatric group of the Italian LIPIGEN (LIPIGEN-FH-PED) and Dutch Lipid Clinic Network (DLCN) criteria. Detailed kindred biochemical and clinical assessments were extended to three generations. The lipid profile was detected by standard laboratory kits, and gene analysis was performed by traditional sequencing or Next-Generation Sequencing (NGS). Results: Among 180 hypercholesterolemic subjects, FH suspected based on the above criteria, 164/180 had the diagnosis confirmed, showing causative mutations. The mutation detection rate (MDR) was 91.1%. The scoring criteria proposed by the EAS, SBR and LIPIGEN-FH-PED (resulting in high probable, possible-defined and probable-defined, respectively) showed high sensitivity (~90%), low specificity (~6%) and high MDR (~91%). It is noteworthy that their application, as a discriminant for the execution of the molecular investigation, would lead to a loss of 9.1%, 9.8% and 9.1%, respectively, of FH-affected patients, as confirmed by the genetic analysis. DLCN criteria, for which LDL-C cut-offs are not specific for childhood, would lead to a loss of 53% of patients with mutations. Conclusions: In the pediatric population, the combination of LDL-C ≥95th percentile in the proband and the dominant inheritance pattern of hypercholesterolemia, with LDL-C ≥95th percentile in one parent, is a simple, useful and effective diagnostic criterion, showing high MDR. This pattern is crucial for early FH diagnosis. EAS, SBR and LIPIGEN-FH-PED criteria can underestimate the real number of patients with gene mutations and cannot be considered strictly discriminant for the execution of molecular analysis.
Full article
(This article belongs to the Special Issue Cardiovascular Disease Epidemiology: A Themed Issue in Honor of Dr. Alessandro Menotti on the Occasion of His 90th Birthday)
Open AccessReview
Non-Pharmacological Treatment of Heart Failure—From Physical Activity to Electrical Therapies: A Literature Review
by
Antonio Scarà, Zefferino Palamà, Antonio Gianluca Robles, Lorenzo-Lupo Dei, Alessio Borrelli, Federico Zanin, Leonardo Pignalosa, Silvio Romano and Luigi Sciarra
J. Cardiovasc. Dev. Dis. 2024, 11(4), 122; https://doi.org/10.3390/jcdd11040122 - 17 Apr 2024
Abstract
►▼
Show Figures
Heart failure (HF) represents a significant global health challenge that is still responsible for increasing morbidity and mortality despite advancements in pharmacological treatments. This review investigates the effectiveness of non-pharmacological interventions in the management of HF, examining lifestyle measures, physical activity, and the
[...] Read more.
Heart failure (HF) represents a significant global health challenge that is still responsible for increasing morbidity and mortality despite advancements in pharmacological treatments. This review investigates the effectiveness of non-pharmacological interventions in the management of HF, examining lifestyle measures, physical activity, and the role of some electrical therapies such as catheter ablation, cardiac resynchronization therapy (CRT), and cardiac contractility modulation (CCM). Structured exercise training is a cornerstone in this field, demonstrating terrific improvements in functional status, quality of life, and mortality risk reduction, particularly in patients with HF with reduced ejection fraction (HFrEF). Catheter ablation for atrial fibrillation, premature ventricular beats, and ventricular tachycardia aids in improving left ventricular function by reducing arrhythmic burden. CRT remains a key intervention for selected HF patients, helping achieve left ventricular reverse remodeling and improving symptoms. Additionally, the emerging therapy of CCM provides a novel opportunity for patients who do not meet CRT criteria or are non-responders. Integrating non-pharmacological interventions such as digital health alongside specific medications is key for optimizing outcomes in HF management. It is imperative to tailor approaches to individual patients in this diverse patient population to maximize benefits. Further research is warranted to improve treatment strategies and enhance patient outcomes in HF management.
Full article
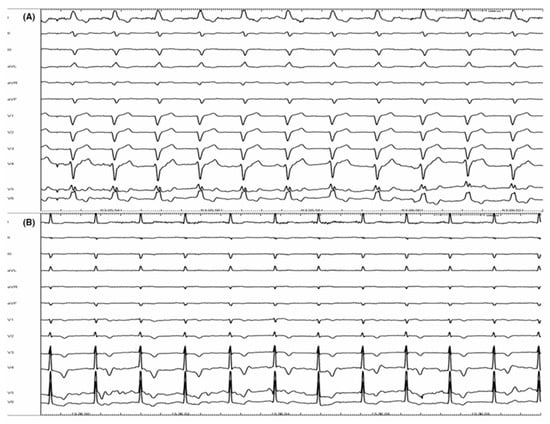
Figure 1
Open AccessArticle
Inflammatory Cells in Adipose Tissue and Skeletal Muscle of Patients with Peripheral Arterial Disease or Chronic Venous Disease: A Prospective, Observational, and Histological Study
by
Joana Ferreira, Adhemar Longatto-Filho, Julieta Afonso, Susana Roque, Alexandre Lima Carneiro, Isabel Vila, Cristina Silva, Cristina Cunha, Amílcar Mesquita, Jorge Cotter, Margarida Correia-Neves, Armando Mansilha and Pedro Cunha
J. Cardiovasc. Dev. Dis. 2024, 11(4), 121; https://doi.org/10.3390/jcdd11040121 - 16 Apr 2024
Abstract
►▼
Show Figures
The main goal of this study was to assess whether the presence of peripheral arterial disease (PAD) correlates with increased inflammatory cell infiltration. An observational, single-centre, and prospective study was conducted from January 2018 to July 2022. Clinical characteristics and anthropometric measures were
[...] Read more.
The main goal of this study was to assess whether the presence of peripheral arterial disease (PAD) correlates with increased inflammatory cell infiltration. An observational, single-centre, and prospective study was conducted from January 2018 to July 2022. Clinical characteristics and anthropometric measures were registered. Consecutive PAD patients with surgical indications for a common femoral artery approach and patients with varicose veins with an indication for surgical ligation of the saphenofemoral junction were included. In both groups, samples of sartorius skeletal muscle, subcutaneous adipose tissue (SAT), and perivascular adipose tissue (PVAT) were collected from the femoral region. We analysed the characteristics of adipocytes and the presence of haemorrhage and inflammatory cells in the samples of PVAT and SAT via haematoxylin–eosin staining. We found that patients with PAD had significantly more inflammatory cells in PVAT [16 (43.24%) vs. 0 (0%) p = 0.008]. Analysing SAT histology, we observed that patients with PAD had significantly more CD45+ leucocytes upon immunohistochemical staining [32 (72.73%) vs. 3 (27.27%) p = 0.005]. Upon analysing skeletal muscle histology with haematoxylin–eosin staining, we evaluated skeletal fibre preservation, as well as the presence of trauma, haemorrhage, and inflammatory cells. We registered a significantly higher number of inflammatory cells in patients with PAD [well-preserved skeletal fibres: PAD = 26 (63.41%) vs. varicose veins = 3 (37.50%) p = 0.173; trauma: PAD = 4 (9.76%) vs. varicose veins = 2 (25.00%) p = 0.229; haemorrhage: PAD = 6 (14.63%) vs. varicose veins = 0 (0%) p = 0.248; inflammatory cells: PAD = 18 (43.90%) vs. varicose veins = 0 (0%) p = 0.018]. Patients with PAD had a higher number of inflammatory cells in skeletal muscle and adipose tissue (PVAT and SAT) when compared with those with varicose veins, emphasizing the role of inflammation in this group of patients.
Full article
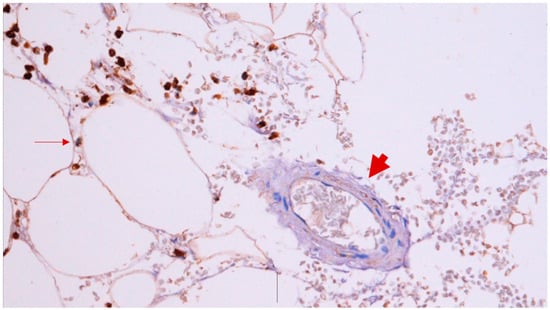
Figure 1
Open AccessArticle
Outcomes of Patients with Normal LDL-Cholesterol at Admission for Acute Coronary Syndromes: Lower Is Not Always Better
by
Ivana Jurin, Anđela Jurišić, Igor Rudež, Ena Kurtić, Ivan Skorić, Tomislav Čikara, Tomislav Šipić, Diana Rudan, Šime Manola and Irzal Hadžibegović
J. Cardiovasc. Dev. Dis. 2024, 11(4), 120; https://doi.org/10.3390/jcdd11040120 - 15 Apr 2024
Abstract
Background and aim: There are few prospective data on the prognostic value of normal admission low-density lipoprotein cholesterol (LDL-C) in statin-naïve patients with acute coronary syndromes (ACS) who are treated with a preemptive invasive strategy. We aimed to analyze the proportion of patients
[...] Read more.
Background and aim: There are few prospective data on the prognostic value of normal admission low-density lipoprotein cholesterol (LDL-C) in statin-naïve patients with acute coronary syndromes (ACS) who are treated with a preemptive invasive strategy. We aimed to analyze the proportion of patients with normal LDL-C at admission for ACS in our practice, and their characteristics and clinical outcomes in comparison to patients with high admission LDL-C. Patients and methods: Two institutions’ prospective registries of patients with confirmed ACS from Jan 2017 to Jan 2023 were used to identify 1579 statin-naïve patients with no history of prior coronary artery disease (CAD), and with available LDL-C admission results, relevant clinical and procedural data, and short- and long-term follow-up data. Normal LDL-C at admission was defined as lower than 2.6 mmol/L. All demographic, clinical, procedural, and follow-up data were compared between patients with normal LDL-C and patients with a high LDL-C level (≥2.6 mmol/L) at admission. Results: There were 242 (15%) patients with normal LDL-C at admission. In comparison to patients with high LDL-cholesterol at admission, they were significantly older (median 67 vs. 62 years) with worse renal function, had significantly more cases of diabetes mellitus (DM) (26% vs. 17%), peripheral artery disease (PAD) (14% vs. 9%), chronic obstructive pulmonary disease (COPD) (8% vs. 2%), and psychological disorders requiring medical attention (19% vs. 10%). There were no significant differences in clinical type of ACS. Complexity of CAD estimated by coronary angiography was similar between the two groups (median Syntax score 12 for both groups). There were no significant differences in rates of complete revascularization (67% vs. 72%). Patients with normal LDL-C had significantly lower left ventricular ejection fraction (LVEF) at discharge (median LVEF 52% vs. 55%). Patients with normal LDL-C at admission had both significantly higher in-hospital mortality (5% vs. 2%, RR 2.07, 95% CI 1.08–3.96) and overall mortality during a median follow-up of 43 months (27% vs. 14%, RR 1.86, 95% CI 1.45–2.37). After adjusting for age, renal function, presence of diabetes mellitus, PAD, COPD, psychological disorders, BMI, and LVEF at discharge in a multivariate Cox regression analysis, normal LDL-C at admission remained significantly and independently associated with higher long-term mortality during follow-up (RR 1.48, 95% CI 1.05–2.09). Conclusions: A spontaneously normal LDL-C level at admission for ACS in statin-naïve patients was not rare and it was an independent risk factor for both substantially higher in-hospital mortality and mortality during long-term follow-up. Patients with normal LDL-C and otherwise high total cardiovascular risk scores should be detected early and treated with optimal medical therapy. However, additional research is needed to reveal all the missing pieces in their survival puzzle after ACS—beyond coronary anatomy, PCI optimization, numerical LDL-C levels, and statin therapy.
Full article
(This article belongs to the Topic Cardiovascular Disease in 2023: Coronary Syndrome, Heart Failure and Structural Heart Disease)
►▼
Show Figures
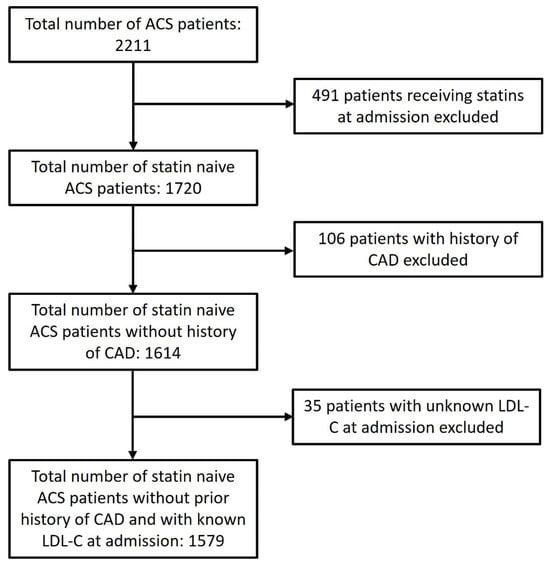
Figure 1
Open AccessReview
Special Considerations for Advanced Heart Failure Surgeries: Durable Left Ventricular Devices and Heart Transplantation
by
Armaan F. Akbar, Alice L. Zhou, Annie Wang, Amy S. N. Feng, Alexandra A. Rizaldi, Jessica M. Ruck and Ahmet Kilic
J. Cardiovasc. Dev. Dis. 2024, 11(4), 119; https://doi.org/10.3390/jcdd11040119 - 15 Apr 2024
Abstract
Heart transplantation and durable left ventricular assist devices (LVADs) represent two definitive therapies for end-stage heart failure in the modern era. Despite technological advances, both treatment modalities continue to experience unique risks that impact surgical and perioperative decision-making. Here, we review special populations
[...] Read more.
Heart transplantation and durable left ventricular assist devices (LVADs) represent two definitive therapies for end-stage heart failure in the modern era. Despite technological advances, both treatment modalities continue to experience unique risks that impact surgical and perioperative decision-making. Here, we review special populations and factors that impact risk in LVAD and heart transplant surgery and examine critical decisions in the management of these patients. As both heart transplantation and the use of durable LVADs as destination therapy continue to increase, these considerations will be of increasing relevance in managing advanced heart failure and improving outcomes.
Full article
(This article belongs to the Special Issue Risk Factors and Outcomes in Cardiac Surgery)

Journal Menu
► ▼ Journal Menu-
- JCDD Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
JCDD, JCM, Medicina, Membranes, ARM
Extracorporeal Membrane Oxygenation (ECMO)
Topic Editors: Patrick Honore, Isabelle MichauxDeadline: 30 November 2024
Topic in
Antioxidants, Biomolecules, JCDD, Metabolites, Neurology International, Pharmaceutics
Tissue-Specific, Disease-Signatured Macrophages in Control of Redox and Antioxidation in Metabolic Diseases
Topic Editors: Xiangwei Xiao, Yingmei Feng, Zhiyong LeiDeadline: 5 July 2025

Conferences
Special Issues
Special Issue in
JCDD
Ventricular Arrhythmias: Epidemiology, Diagnosis and Treatment
Guest Editors: Antonio Di Monaco, Massimo GrimaldiDeadline: 30 April 2024
Special Issue in
JCDD
Diseases of the Aortic Valve and Ascending Aorta: An Overview of Current Knowledge on Pathogenesis, Diagnosis and Treatment
Guest Editors: Francesco Nappi, Ivan Carmine GambardellaDeadline: 15 May 2024
Special Issue in
JCDD
Transcatheter Aortic Valve Implantation (TAVI) II
Guest Editors: Enrico Ferrari, Sergio BertiDeadline: 31 May 2024
Special Issue in
JCDD
Biophysical- and Engineering-Oriented Approaches to Energy-Based Cardiac Ablation Techniques
Guest Editors: Ana González-Suárez, Erik B. Kulstad, Juan J. Pérez, Ramiro Miguel IrastorzaDeadline: 15 June 2024









